Deep Brain Stimulation Surgery for Parkinson’s Disease Motor Symptoms (DBS Surgery)
This post is to share our family’s experience with deep brain stimulation surgery for Parkinson’s disease (DBS) and is not intended as medical advice. Please discuss your symptoms with your neurologist for medical advice.
Deep Brain Stimulation Treatment for Parkinson’s Disease
It has been a while since I have posted about my husband’s battle with Parkinson’s disease. He was first diagnosed with Parkinson’s in January 2022. The symptoms were subtle at first. When we began to suspect Parkinson’s disease, we saw his primary care physician, who then referred him to neurology at the University of Utah Hospital. For a while there, we saw a lovely nurse practitioner, but as his Parkinson’s symptoms advanced, she eventually referred us to one of the neurologists at the University of Utah Movement Disorders Clinic. His motor symptoms were fairly well controlled for a while on medications, but as they increased we began to consider the option of deep brain stimulation surgery for him. The goal of the deep brain stimulation surgery is to reduce motor symptoms such as tremors and muscle stiffness.
DBS Surgery Stages
Deep brain stimulation surgery is a two part surgery. During the first surgery the neurosurgeon places wires into the brain. During the second surgery, the neurosurgeon attaches extensions to the wires that then attach to an impulse generator, which was placed under the skin in his chest during that same surgery.
Deep Brain Stimulation Stage 1
Dave’s first phase of DBS placement was scheduled to be done in February, 2025. We had meticulously scheduled the two phases of the surgery and all of the imaging, office, and lab visits associated with it around a trip we planned for the end of March to go see family in Iowa and Illinois. That plan had to change when Dave cut off the end of his middle finger accidentally on Valentine’s Day. Because it was a large wound and there was risk of infection, the neurosurgeon did not feel comfortable moving forward with an elective surgery (DBS) until his finger was well on its way to healing.
Surgery was rescheduled. Phase one to be done on April 16 and phase two to be done on April 30. On April 16, we checked in at the University of Utah hospital and went to the surgery department.
After they got Dave all ready for surgery, consents for treatment were signed, and they wheeled him away to the operating room. The neurosurgeon told me the first surgery could be 2-4 hours long and after that he would be in the recovery room for a couple of hours before I could see him, so I prepared for the long wait. I did my best to keep myself busy working on my computer in order to keep my mind off of the fact that someone was drilling into my husband’s skull not to far away from me.
After about an hour and a half the doctor came out and told me surgery went well and they would be moving Dave to recovery. Once they moved Dave from the recovery room to his room on the Acute Neurology floor, I would be able to be with him. That ended up being at almost 7 o’clock at night and by then, I’m not going to lie-I was getting a bit irritable about not being able to be with my husband. Eventually, I was able to meet him in his patient room and spend some time with him before I went home to be with our teenager. All in all, he came through the first surgery okay. He felt unsteady the first couple of days, but his incisional pain was pretty manageable. He had two incisions on top of his head, through which they drilled through his skull so that they could introduce the DBS wires into Dave’s brain. The doctor said the actual drill holes in the skull were only about 3 mm wide and they would close up on their own over time. The surplus length of the initial two wires were coiled under the skin on top of Dave’s head until the second surgery.
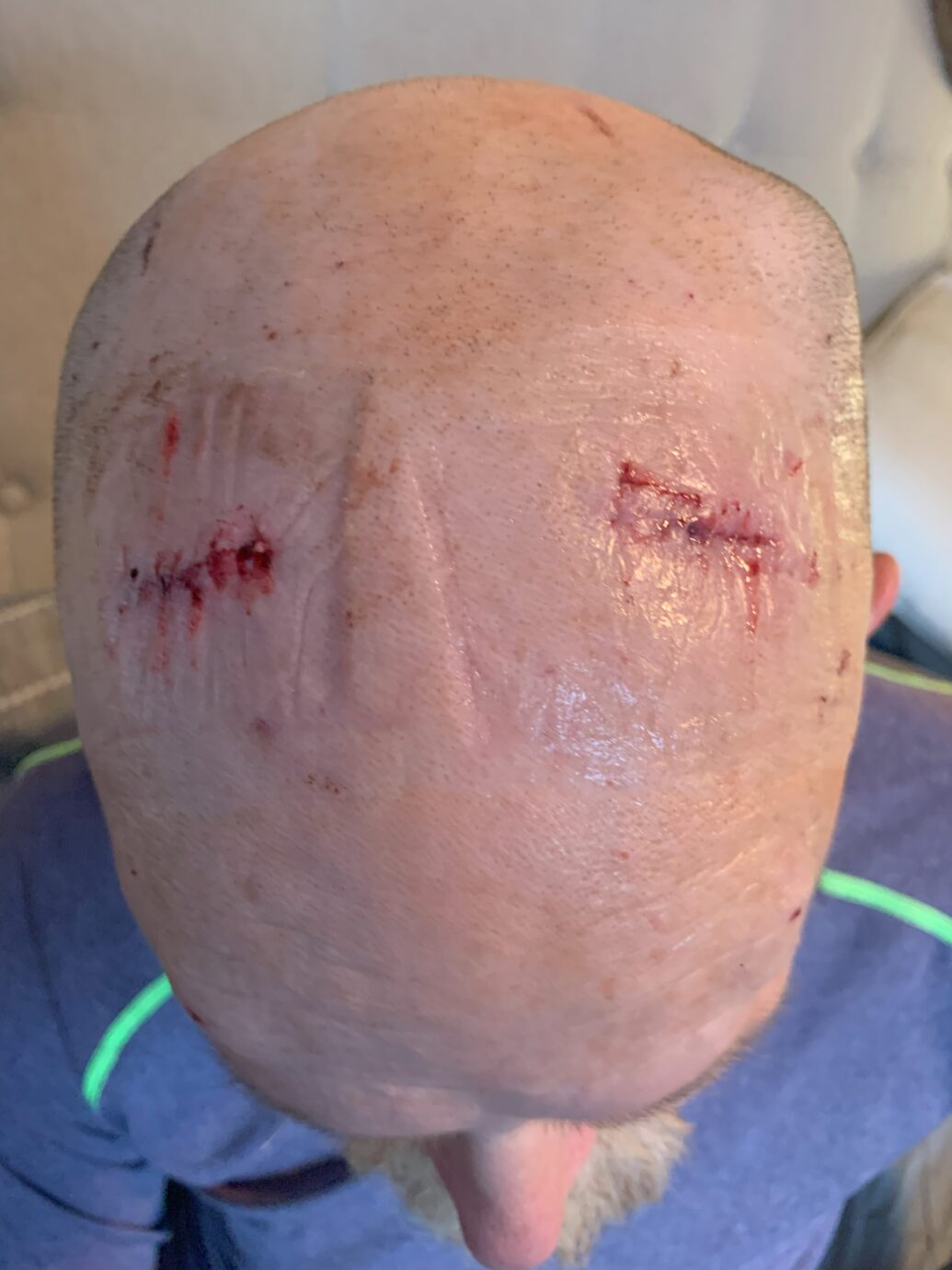
When he was sent home from the hospital the next day, he was instructed not to lift anything heavier than a jug of milk or do any vigorous exercise for a month (because these instructions would extend through two weeks after the second surgery). At home, we were able to take off the dressing and see the incisions (not to mention the goose egg back where the coiled wires were.
Six days after the first DBS surgery, Dave felt well enough to go see one of our kiddos in a school play!

Eight days after the first DBS surgery, Dave was feeling well enough to go to Cedar City to see our daughter, Annie, graduate from Southern Utah University!

Deep Brain Stimulation Surgery Stage 2
The second phase of Dave’s DBS surgery was on April 30. Dave was taken to the operating room from pre-op around 2:30 in the afternoon and after about an hour the neurosurgeon came out to talk to me. He told me everything in surgery went well and they turned on the DBS device briefly to confirm it was functional. They then turned it off, as it would remain until his upcoming appointment to have it programmed with his neurologist on May 9. That has not happened yet, but I will write about it when it does and link it to this page.
While Dave was in the post-anesthesia care unit recovering from the second surgery, the product representative from the DBS device manufacturer came out to the waiting room to give me some supplies and review the basics of how to use the device, so that I could teach Dave when he woke up. The machine wasn’t getting turned on just yet, like I said previously, but at least it gave us a general idea of what to expect. I plan to write a separate post about the deep brain stimulation device itself, which I will link to this article when it is done.
For Dave, this surgery was more uncomfortable post-op than the first one. He had a new incision in his head, where they attached extenders to the wires, which they threaded down through his neck (under the skin), plus a new incision in his chest, where the impulse generator was placed. The good thing was he didn’t have the unsteadiness he had after the first surgery.
What is Life Like After DBS Surgery?
In my next post about our journey with DBS surgery and Parkinson’s disease, I will share details of the process of training the DBS device. I hope that if you or your loved one are considering deep brain stimulation surgery for Parkinson’s disease, this has helped you to feel more informed about what you can expect if you choose to proceed. If you have questions, feel free to drop them in the comments. My husband and I are very open about his Parkinson’s Disease journey and we will be happy to answer questions.
See you next time!
Debra



3 Responses